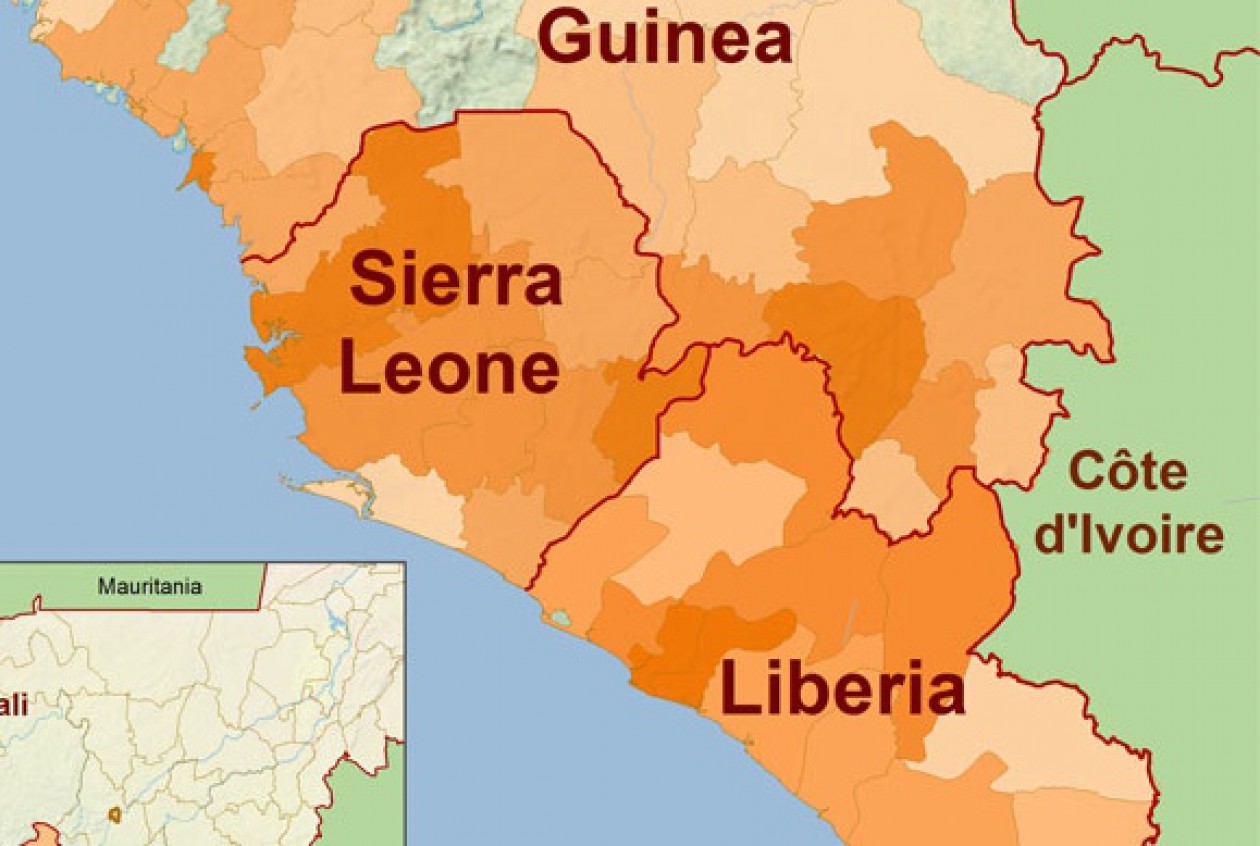
**For some context, in November of 2014 the Ebola Treatment Unit (ETU) we worked in had the highest census of the entire time it was open; we were overwhelmed with patients from three different Ebola hotspots exacerbating the epidemic within about a 6 hour ambulance drive from our ETU. Throughout the time IMC ran ETUs (and other organizations as well), there was a constant effort to improve treatment and quality of care. But the limitations were extraordinary–very little was known about what treatments would be efficacious against Ebola, it was difficult to access or import needed medications and equipment, direct patient care time was limited by the short duration of time one could safely work in hot conditions while wearing PPE . . . it was hard. In hindsight, we learned a lot, there are things we would change if given a chance to go back, and we hope that data that is being analyzed even now will shed more light on how to better treat Ebola next time it rears its ugly head.**
This month of stopping, of coming off the adrenaline-driven 14 months of working to fight Ebola in Liberia, has finally granted the space and time to process much of what happened during that time. In the middle of sweating through a shift at the Ebola Treatment Unit or preparing for marathon Ministry of Health meetings or painstakingly reviewing budgets at midnight–there wasn’t time to process much of the emotions of any of it. Those had to be pushed to the side, compartmentalized into a corner of our minds and hearts so we could just cope and keep going. This is the reality of an emergency, but not a healthy long-term method of coping. So I expected to begin to remember, to think, to feel in these weeks. But nothing prepares you for loss and grief, no matter how professional and clinical and ‘used to it’ you are.
Journal Entry, November 2014
J. should not have died. I’m convinced that ultimately it was not Ebola that killed him; rather it was the awful reality that no one had the time (or PPE endurance) to sit and hold him and coax fluids into his weak and tired body. He lost so much, and my heart broke to hear his whimpers and see his floppy body on that bed all alone {baby J lost multiple family members to Ebola, several in our ETU}. I wish I’d started sooner, I’d taken more time for him–I wish everyone had.
But on the {ETU} ward there is precious little time to do what needs to be done, and the loudest voices (or vomiting) get the most attention.
In a crisis, there is little else you can do.
But it’s still so wrong.
I tried to block the memories for a long time, but I remember.
I remember picking up this precious child one afternoon on my shift in the ETU confirmed ward, from his mattress on the cement floor. He was so weary, so sick, his body worn out from fighting and losing so much. I held him, and he flopped his little head against my breast. Only, he couldn’t really feel me, through the layers of my heavy vinyl apron and my PPE suit and scrubs and three pairs of gloves. And he couldn’t really hear me, through my hood and two masks. And he couldn’t see me, through my sweaty and fogged up goggles. I slowly squirted ORS from a syringe into his mouth, tried to patiently wait for him to swallow. Heard the calls of the clinical team needing help with other patients. Knew he needed someone with him all the time, to give him more than a few cc’s of fluids, to hold and comfort him, to tell him he was beautiful and precious and worthy and so very loved. And I couldn’t stay. I couldn’t be that person–our time inside the unit for that round was almost up, measured by the amount of sweat filling our boots and how little we could see out of our goggles and our shallow breaths taken against sweat-soaked masks. I prayed over him, sang over him, laid him on that forlorn mattress all alone on the floor. I resolved to prioritize his care and ask a couple other clinical team members to do the same on our next shifts inside the unit.
Baby J. died that evening, alone, before I got a chance to go back into the Ebola confirmed ward.